After Colon Surgery

You may not remember the recovery room (Post-anesthesia Care Unit or PACU) after anesthesia, but after your surgery, expert nurses will watch you closely until you are transferred to the floor.
A nurse will be at your bedside monitoring your recovery while you wake up. You will see machines checking your heart, your blood pressure, and your breathing. You will be reminded to take deep breaths after you wake up. The inflatable massaging leg coverings will still be on your legs. Your family/friends will be updated by the nurse in the PACU.
Nursing Unit
You will be moved to the nursing unit with intravenous (IV) fluids, a catheter in your bladder and a bandage on the abdomen. You may have also have oxygen and a pain medication pump. On arrival to the unit a nurse and care technician will continue to monitor your recovery and your nurse will begin your postoperative plan. Your family will be able to be at the bedside after you are checked in on the nursing unit.
Your Team
At the beginning of this book, you read about the multidisciplinary team model; which means that experts from throughout the hospital will support your recovery before, during, and after your surgery. They will work together to watch how you are recovering and plan the best steps for your recovery. These people will support and teach you how to carry out the activities that will help you recover better and faster.
You will also have a Care Management team, which consists of an RN Case Manager and a Social Work/Discharge Planner. This team, working with your doctor and nurse, will identify your recovery needs in the hospital and beyond our walls. They will provide you with the best discharge plan possible to meet your post-hospital needs for recovery.
Your patient care team will help you by focusing on three important parts of your recovery plan:
- Eating and drinking
- Activity
- Pain management
The most important members of your recovery team are you and your family since it is up to you and them to help carry out this plan. Your designated healing partner should plan to be at the bedside the remainder of the afternoon/evening. Please limit family/visitors to one or two people.
What Happens After Surgery?
The goal after surgery is to restore your normal body functions as soon as possible. Your team will make changes to fit your special needs.
Eating and Drinking
Soon after surgery you may be given clear liquids to drink if ok with your surgeon. Drinking liquids soon after your surgery can help your bowels return to normal function. Since getting air in your bowel may cause bloating and nausea, carbonated drinks (like soda) and straws are not allowed.
Activity
You can expect to get out of bed on the day of your surgery. This can mean standing, sitting in a chair, walking, or a mixture of these things. If you arrive in your room before 2 p.m., you can expect to be out of bed at least 2 times on the day of surgery. You will be in a chair for meals. Over the following days, you will be asked to spend more and more time out of bed. Your nurses will help you set goals for the amount of time spent out of bed. They will show your Healing Partner how and when to help you with your activity.
Pain Management
Options will be thoroughly discussed with you, including the benefits and risks. No surgery is pain-free. Your doctors will decide how to best manage your pain. Several methods will be used to manage your pain. These may include :
- Intravenous (IV) pain medication
- Pills for pain
- A button to control your pain (PCA pump)
- An epidural catheter (a catheter that delivers continuous pain medication into your back); this usually continues for 24-36 hours after surgery
- Regional block (injection of numbing medicine into your abdominal wall)
Rating your pain is important. It lets your team know how much pain you are feeling so that adjustments can be made to your medication. Memorial Hospital uses a pain scale of 0 to 10. A pain rating of 0 means you have no pain while a rating of 10 means the pain is the worst possible.
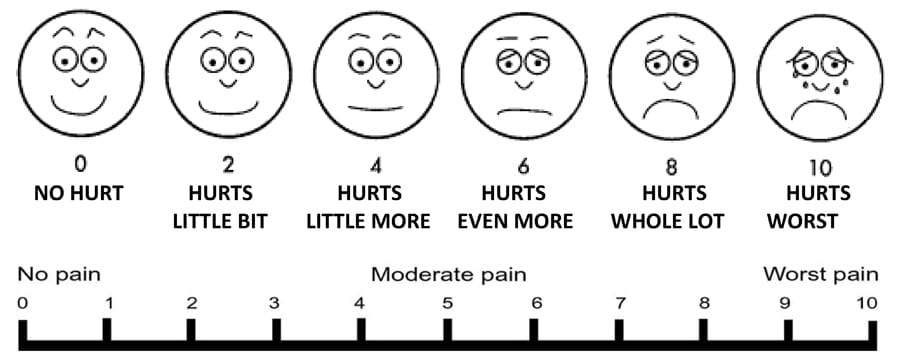
Your care team will help you set a target pain level. This target is a level of pain you can tolerate so you can continue the recovery activities of deep breathing and getting out of bed. Your nurse will assess your target pain level every shift.
Breathing Exercises
Remember the deep breathing exercises you read about during your pre-admission visit? Your Healing Partner should remind you to do your cough and deep breathing exercises every hour while awake. A nurse will bring you a device called an incentive spirometer and show you how to use it to help keep your lungs clear. Both you and your Healing Partner will learn how you can best use this breathing tool.
Blood clot prevention
While you are in bed, you can help prevent blood clots by doing ankle pumps every hour or two while you are awake. To perform ankle pumps, move your ankles up and down 10 times. The inflatable massaging leg coverings will gently squeeze and massage your lower legs to prevent blood clots. These will stay on until you spend most of your day out of bed.
Other Things to Expect
Everyone who may touch you or anything in your room should wash their hands or use hand sanitizer first. This includes all visitors. Avoid touching your incision, but if you do, use hand sanitizer first.